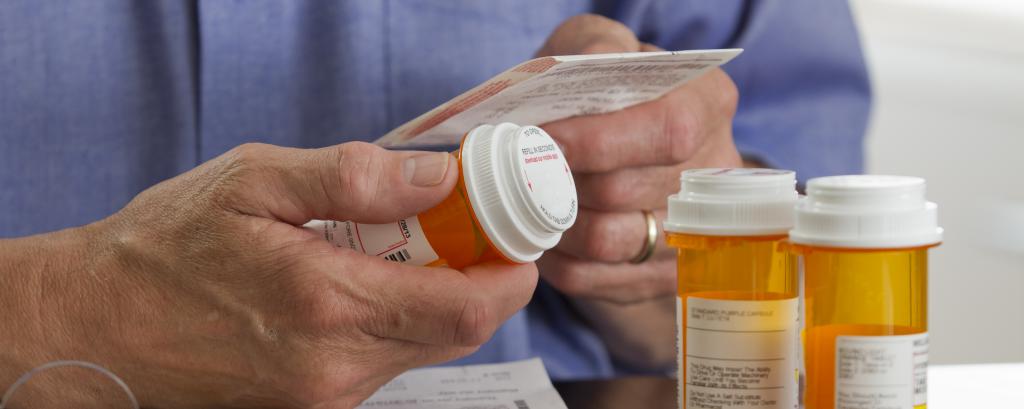
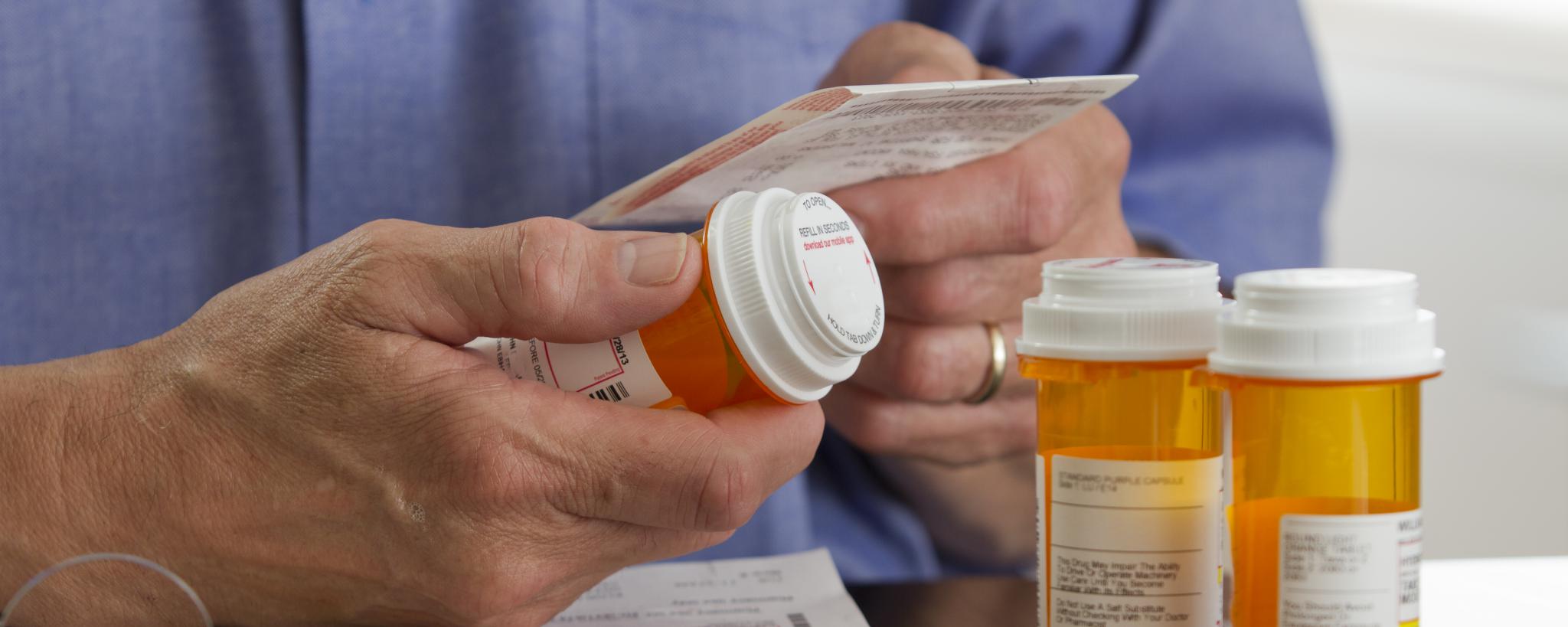
The continuously increasing computer resources, growing data repositories, and improving pattern-learning algorithms has recently triggered a new trend in medicine: the wish to go from “population medicine” to “personalized medicine”.
“From #populationMedicine to #personalizedMedicine using fine-grained stats.“
Twittern WhatsApp
Historically, new treatment is developed in medicine by recourse to its effectiveness in the population as unit of observation. It tries to answer which drug or treatment plan works best for the majority of the many different people of the population. In this context, two facts are common knowledge to virtually every medical doctor. First, until about 1900, the life expectancy of a person consulting and following the advice of a medical doctor did actually decrease, not increase! Second, even at the beginning of the 21st century, most treatments do only show beneficial effects in a fraction of the patients for whom that treatment is indicated and (perhaps even daily) administered.
However, the big-data era has changed the granularity of the questions about personalized treatment that we can ask in both medical research and practice. More precisely, it is becoming increasingly possible to ask, quantify, and predict how well a given treatment works in a new observation unit: the single individual. This opens the window of opportunity to actually design and administer treatment plans that are individualized for and optimized to every person seeking medical attention. As a first example, if the genetic equipment of an individual contains a gene variant that prevails a positive outcome of taking the usual first-choice drug A, the medical system can not only save costs but also increase the patient’s well-being by directly prescribing an alternative drug B. As a second example, drug treatment of psychiatric patients is still today to some extent based on trial and error and typically takes several weeks to show a positive or negative effect. The possibility of person-specific prediction of potential drug response could reduce prolonged suffering of these patient populations and their families.
Conclusion
The possibility of personalized prediction in medicine is likely to have a long-lasting impact on how clinical research is conducted by scientists and how medical care is provided by health professionals.
Learn more: